The Duke Liver Transplant Program this spring marks 2,000 transplants with patient outcomes that are among the best in the nation for key metrics such as shorter transplant wait times and one-year survival.
While median wait time for a liver transplant in the U.S. is about 240 days, Duke’s wait time is 85 days. The median one-year liver transplant survival rate from deceased donors is about 95.92 percent at Duke versus 91.89 percent for the country.
From one transplant in 1984 to 123 transplants in 2022, the Liver Transplant Program’s growth and success has come largely under the leadership of Professor of Surgery and Pediatrics Deb Sudan, MD, chief of the division of Abdominal Transplant in the Department of Surgery, and Carl Berg, MD, professor in the division of Gastroenterology. The partnership between Medicine and Surgery has made Duke the high-volume, high quality transplant center that it is today.
Sudan joined the program in 2008, recruiting and establishing a stellar team of highly-skilled surgeons capable of performing technically-complex transplants and establishing a track record of success. The program volume doubled, going from 30 to 60 transplants annually with survival outcomes among the highest in the country. Duke also started consistently doing between 10 and 20 pediatric liver transplants per year after Sudan’s arrival—a dramatic increase in that offering for North Carolina patients.
Berg came on board in 2012 with a directive to further grow the program.

“Our success represents the culmination of a lot hard work by literally dozens of disciplines that work together and think outside the box, which is a characteristic of our program,” said Berg, who passed the director’s baton in October 2022 to hepatologist Lindsay King, MD, MPH, assistant professor in the division of Gastroenterology. “Through expanding our organ pool with hepatitis C and hepatitis B virus positive organs and expansion of the use of donation after circulatory death livers, we have been able to transplant a larger number of patients.”
“We have a top tier program because of the coordinated efforts of multiple team members and a supportive hospital administration,” said King. “Our outcomes are higher than national outcomes and higher than expected for the population that we treat because we really have a great multidisciplinary team and excellent communication between our surgeons and hepatologists and a program focused on providing high quality care.”
Better surgical techniques and immunosuppression for liver transplant procedures have improved since the Duke Liver Transplant Program was started in the mid-1980s, also playing a role in the program’s growth, as has expansion of the donor pool with the addition of organs from patients with hepatitis C and hepatitis B virus infections. Sudan notes that Andrew Muir, MD, MHS, and the Duke Clinical Research Institution are two of the national leaders responsible for getting the drugs that are effective for hepatitis C to market.
Donor livers now can also be preserved longer now with perfusion devices that circulate oxygenated blood through the organ so it can travel farther to recipients. Duke’s surgical team has been one of the largest enrollers for new perfusion devices, which allows for the use of organs that otherwise would have injury from preservation.
“One of the things we feel very strong about as a team is trying to be sure that every patient who has liver disease has access to care for their liver disease, and an opportunity to undergo transplant when they need it,” Sudan said. “I think what our 2,000 milestone represents is the fact that we are committed to increasing access to transplantation for our patients and providing them with the care they need when they need it."
The Duke Difference
With liver transplant surgeons among the most experienced in the nation, Duke’s transplant teams have the capacity to perform liver transplants on patients with complex medical or surgical conditions and relatively rare multi-organ transplants—including heart-liver, liver-lung, and liver-small bowel-pancreas. In 2021, Duke was among the top 10 institutions in the nation to perform multi-organ transplants.
Chronic liver disease patients at Duke also benefit from split liver transplants divided between two people—a transplant that few other programs offer due to the level of technical difficulty and depth or size of the surgical team needed to do simultaneous transplants.
Duke also has a solid organ transplant unit that is dedicated to caring for transplant patients with a team of multidisciplinary caregivers that includes doctors, nurses, pharmacists, social workers, patient coordinators, consulting providers and more. Duke’s commitment to care also begins with organ disease, before the time of transplantation, and extends to post-operative care.
A new area of growth is living donor liver transplants, where diseased or injured livers are replaced in part or portion with livers from healthy donors. The goal is to ensure that patients with end-stage liver disease get timely referrals to transplant and expand the program’s catchment area, which is mainly the Southeast and North Carolina.
Plans are also being discussed for deeper community outreach to gastroenterology practices and primary care providers and the addition of satellite clinics to help care for patients that live further.
“Transplantation is an ever-evolving field and there's still a supply and demand imbalance for liver transplants,” King says. “There are more people dying of end-stage liver disease and that number grows with the population so we still need to continue to grow to meet the demand.”
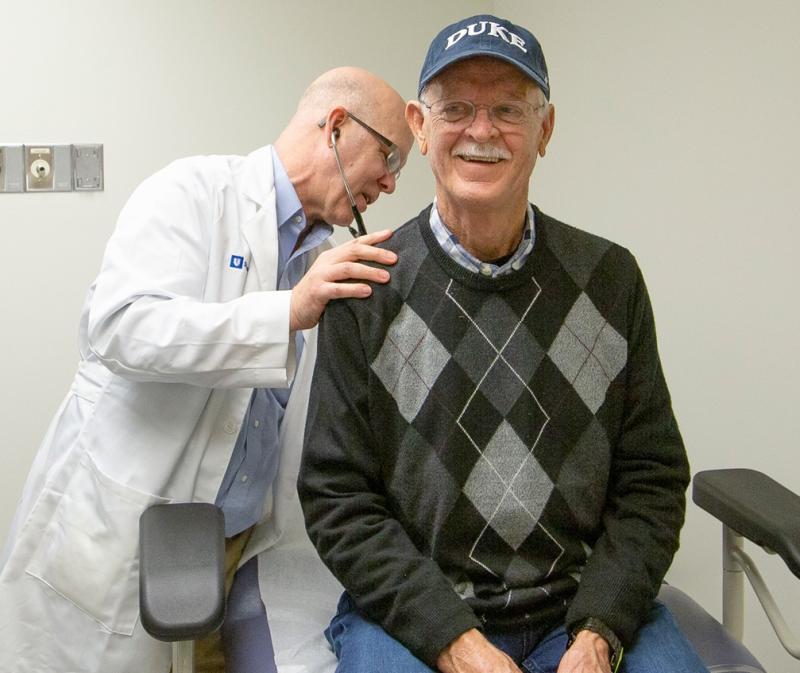
Feature photo: Dr. Carl Berg examines a transplant patient.