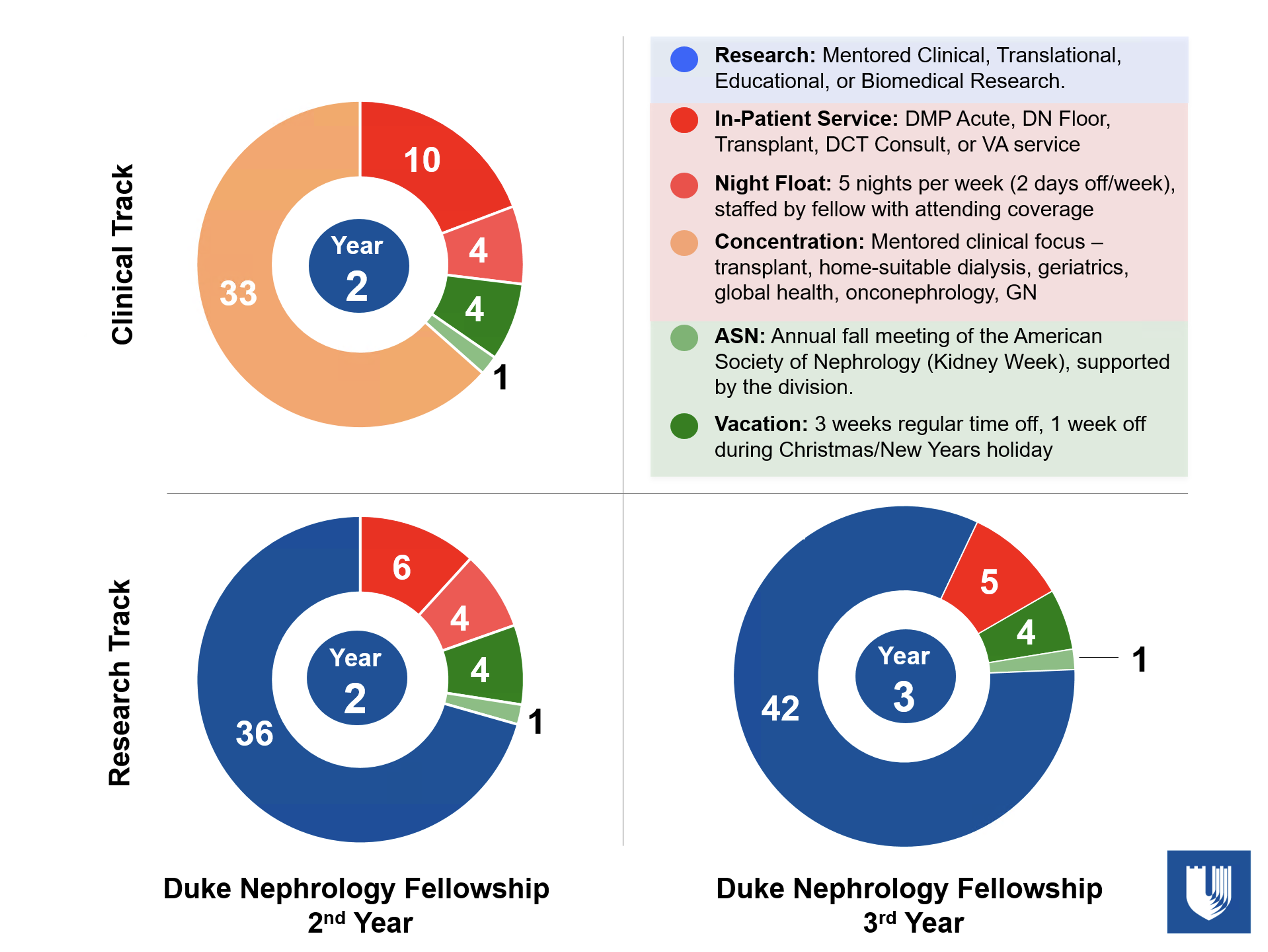
First Year
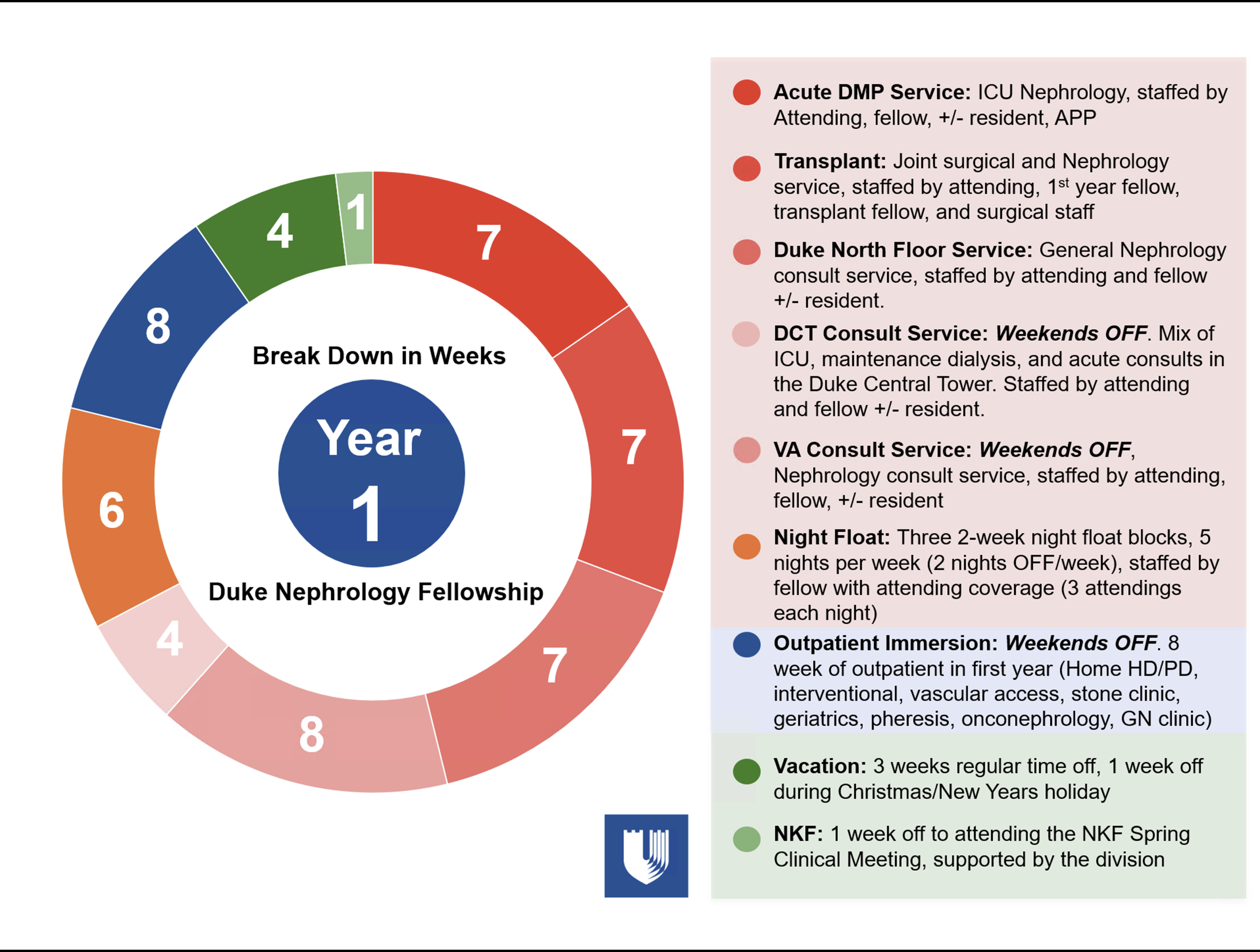
Second and Third Years
Fellow Driven Program Improvement
Work-life balance is a vital pillar of a successful and sustainable career in medicine. To support this, we have established the Fellowship Improvement Committee (FIC), a fellow-led initiative chaired by the Chief Nephrology Fellow and including representation from the first-year fellow class.
The FIC also includes key stakeholders such as Associate Program Directors (APDs), the Program Director (PD), and faculty members across all domains of the program—clinical, research, transplant, and education. The committee meets regularly and reports directly to the Division Chief.
Its mission is to proactively engage with alumni, applicants, faculty, and current fellows to identify and address both current concerns and emerging needs within the fellowship. Through its ongoing efforts, the FIC continues to make a meaningful impact on enhancing the work-life balance and overall experience of our fellows.

Ale Tomasi, MD, chief fellow- Chair, 2nd year fellow
Komal Safdar- 2nd year fellow
Mike Tabet- 1st year fellow
Matthew Sparks, MD- PD
Harpreet Singh, MD- APD
Rasha Raslan, MD- APD
David Ortiz-Melo, MD- Clinical
Susan Murray, MD- Inpatient Dialysis Director
Wissam Kourany, MD- VA Chief
Micah Schub, MD- Transplant

Clinical Inpatient Rotations (all purely consult services)
Clinical Services Overview
| Service | Description |
|---|---|
| Acute (ICU) DMP Nephrology Service | This service provides interventional and consultative nephrology care—including continuous venovenous hemodiafiltration (CVVHDF)—for critically ill patients in the intensive care units of Duke Medicine Pavilion (DMP). It excludes patients with kidney transplants. The team includes a rounding physician extender (PA or NP), ensuring comprehensive and timely care. |
| Duke North Floor Nephrology Service | This consultative service supports patients admitted to the general medicine wards in the North Tower of Duke University Hospital. It excludes patients on maintenance dialysis or with kidney transplants. Fellows gain experience managing a wide range of inpatient nephrology issues in a general medical setting. |
| Transplant Nephrology Service | Fellows on this rotation work one-on-one with a transplant nephrology attending across both inpatient and outpatient settings. Responsibilities include managing all kidney transplant consultations throughout the medical center and performing inpatient transplant kidney biopsies. Fellows also participate in the transplant listing conference and monthly morbidity and mortality (M&M) conferences, ensuring comprehensive exposure to all aspects of kidney transplantation—starting in the first year. |
| Duke Central Tower (DCT) Consult Service | This smaller consultative service provides care for a mix of ICU and floor patients in the Duke Central Tower. It offers a clinical experience reflective of private practice nephrology. Fellows on this service have weekends off, supporting work-life balance. |
| Durham VA Medical Center Nephrology Service | This consultative service at the VA offers a broad range of nephrology experiences, including fluid and electrolyte management, acute and chronic dialysis, transplant follow-up, and general nephrology care. Fellows benefit from a varied patient population and have weekends off during this rotation. |
Ambulatory Clinics and Outpatient Clinical Immersion
During the first two years of fellowship, all fellows participate in a half-day continuity clinic that alternates weekly between Duke and the VA. This structure provides a diverse clinical experience across different healthcare settings.
Third-year research fellows are generally exempt from clinical duties unless specifically requested, allowing them to focus more intensively on their research projects. When clinical involvement is requested, it is closely aligned with their individual research interests.
The Duke Fellows Clinic (1A) is directed by Dr. Sparks, who oversees the educational and clinical components of the fellows’ ambulatory training.

To ensure a robust and immersive outpatient experience, each first-year fellow completes eight weeks of dedicated outpatient rotations, structured as four two-week blocks throughout the year. These rotations provide broad exposure to a variety of ambulatory nephrology settings.
During these outpatient blocks, fellows are not assigned weekend duties, allowing them to focus fully on clinical learning and professional development. One of these weeks is specifically designated for independent study in preparation for the ABIM Internal Medicine Board exam, supporting fellows in achieving board certification.
Additionally, all major presentations—such as Journal Club and Grand Rounds—are scheduled during these outpatient periods. This ensures that fellows are not burdened with presentation responsibilities while managing the demands of inpatient service.

Faculty Lead- Harpreet Singh, MD
Associate Program Director
These rotations can include any of the below:
- Transplant donor and recipient surgery
- Interventional nephrology
- Permanent vascular access creation and maintenance
- Plasmapheresis
- Outpatient management of transplant patients
- Palliative Care
- Nephrolithiasis
- Hypertension Clinic
- Duke Lupus Clinic
Each fellow also participates in an outpatient dialysis rotation (6 months) and attends a monthly peritoneal dialysis clinic during the 2nd year of training.
Individualized Career Development- Scholar Pathways
Clinical Investigator Pathway (3 years)
Biomedical Science Investigator Pathway (3 years)
Clinical Concentration Pathway (2 years)
Global Health Pathway (2-3 years)
What to Expect in the Second Year of the Clinical Concentration Pathway
The Division has a long history of training outstanding physicians in the practice of Nephrology and we actively encourage applicants who desire a career in practice to apply. Clinical fellows will also complete a quality improvement or research project as part of the second year of training. The clinical concentration pathway consists of additional time on the clinical services and potentially elective experience tailored to the interests of the individual with possibilities including
- The Transplant Concentration- Scott Sanoff
- The Geriatric and Palliative Care Concentration- Rasheeda Hall
- Home Suitable Dialysis Concentration- Rebecca Frazier
- Glomerulonephritis Concentration- Harpreet Singh
- Onconephrology Concentration- David Ortiz-Melo
What to Expect in the Second Year and Beyond in the Investigator Pathways
For fellows pursuing an academic career, the second and third years of the fellowship include intensive research training under the direction of a faculty mentor, with multiple sources of funding available including an NIH funded NC KUH TRIO training grant (U2C/TL1), an HSR&D grant through the VA Medical Center, other extramural grants, and endowment sources available to the Division. A mentoring committee is established for each research fellow to assist the primary mentor in guiding the fellow. Additional years of training are often desirable and often available for a small number of outstanding candidates for a career in academic medicine. Fellows can decide to enter this pathway AFTER joining the fellowship program.
Multiple nephrology conferences are available throughout the academic year including journal club, GN club, outpatient conference, board review, nephropathology working rounds conference, clinical and research core curriculum, multidisciplinary conference, and grand rounds. All conferences are recorded, edited and archived.
Several faculty members at Duke continue to independently perform kidney biopsies, reflecting the division’s strong procedural expertise. In addition, the majority of native and transplant kidney biopsies are performed by a dedicated biopsy service led by John Musgrove, MD, ensuring high procedural volume and consistency. This structure provides fellows with ample opportunity to observe, assist with, and ultimately achieve competence in performing kidney biopsies under expert supervision.

John Musgrove, MD
Faculty Lead, Kidney Biopsy
Fellows receive comprehensive training in home dialysis modalities, including Peritoneal Dialysis (PD) and Home Hemodialysis (HHD), as a core component of the fellowship. Our division manages the care of over 120 patients on peritoneal dialysis, offering fellows substantial exposure to this growing area of nephrology.
Dr. Murray and Dr. Lehrich oversee the majority of these patients and play a central role in providing hands-on learning opportunities and mentorship in home dialysis care. Dr. Frazier coordinates the clinical rotations and administers the home dialysis curriculum, ensuring that fellows are actively engaged in all aspects of home therapy, including participation in new patient education sessions and home clinic visits.

Rebecca Frazier, MD
Faculty Lead, Home Dialysis
Point-of-care ultrasound (POCUS) is an essential skill for the modern nephrologist, and our fellowship places strong emphasis on its development. All first-year fellows participate in a dedicated two-week POCUS immersion that combines hands-on scanning sessions with structured didactics.
For those seeking deeper proficiency, a more advanced curriculum is available during the second year, allowing fellows to refine their skills and apply them in more complex clinical scenarios.
Fellows have access to a range of high-quality ultrasound equipment, including handheld Butterfly iQ+ devices for bedside use. Additionally, the division is equipped with Sonosite M-Turbo portable ultrasound systems and Kosmos ultrasound machines at both Duke and the Durham VA. The Kosmos systems feature advanced artificial intelligence capabilities, including automated guidance, anatomical structure labeling, image quality grading, and ejection fraction (EF) calculation, enhancing both learning and diagnostic accuracy.
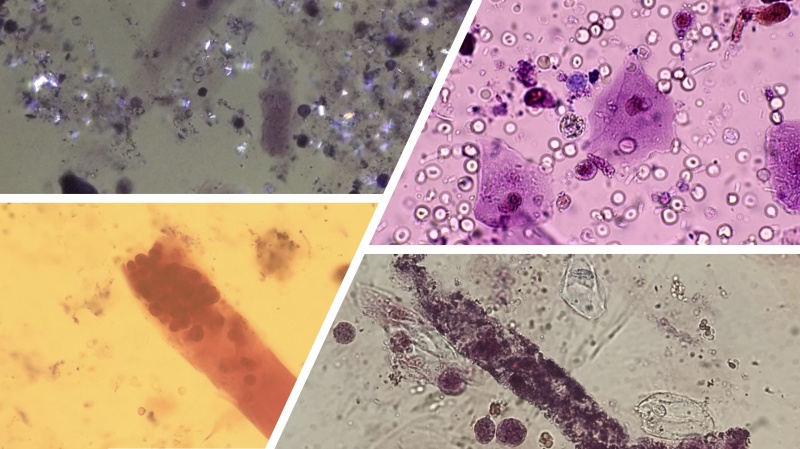
Fellows at Duke receive structured training to develop proficiency in performing and interpreting urine microscopy—an essential diagnostic skill in nephrology. Training includes exposure to multiple microscopy modalities, such as brightfield, phase contrast, darkfield, and stained specimens using Sternheimer-Malbin stain.
To support this hands-on learning, the program provides access to three dedicated microscopes located at key clinical sites: the Durham VA Hospital, the Duke 1A Fellows Clinic, and Duke Hospital for inpatient use. This ensures fellows can integrate urine microscopy into both outpatient and inpatient clinical decision-making.

Fellows at Duke gain exceptional, hands-on experience in kidney transplantation through one of the nation's most established and high-volume transplant centers. Since performing its first kidney transplant in 1965, Duke’s Kidney Transplant Program has completed more than 3,000 transplants, including over 1,000 from living donors. Currently, the program performs approximately 250 kidney transplants annually, making it one of the highest-volume and most experienced centers in North Carolina. The program is supported by a dedicated team of nine full-time transplant nephrologists, ensuring robust clinical mentorship and educational engagement.
Fellows are deeply involved in all facets of transplant nephrology, including comprehensive pre-transplant evaluations, inpatient and outpatient management, individualized immunosuppression strategies, and long-term graft monitoring. Duke also has recognized expertise in complex, multi-organ transplant procedures, offering exposure to combined kidney-liver, kidney-heart, kidney-pancreas, and kidney-small bowel transplants. This rich and diverse clinical experience prepares fellows to confidently manage a wide range of transplant scenarios and positions them for leadership roles in both academic and clinical transplant nephrology.

Micah Schub, MD
Faculty Lead, Transplant
How is Mentorship Provided?
Each fellow at Duke works collaboratively with faculty to establish a personalized Mentorship Committee that supports their academic and professional development throughout the duration of their fellowship. This committee typically includes a primary research mentor and two to three additional faculty members with complementary scientific interests from across Duke University.
The Mentorship Committee meets semi-annually to review the fellow’s progress, discuss short- and long-term goals, clarify expectations, and provide strategic guidance on career development. Following each meeting, the fellow is expected to prepare a written summary outlining key discussion points and action items. This summary is shared with the committee members, the Division Chief, and the Training Program Director to ensure alignment and accountability.
Fellows pursuing the basic science pathway also have the opportunity to join the Lefkowitz Society, which offers additional mentorship, networking, and career development resources tailored to physician-scientists.
Ongoing Quality Improvement Projects
In alignment with ACGME requirements, the Duke Nephrology Fellowship has developed a robust and longitudinal Quality Improvement (QI) program that is integrated into the core training experience. All fellows actively participate in QI initiatives throughout their fellowship, gaining valuable skills in systems-based practice, patient safety, and data-driven clinical improvement.
For fellows with a strong interest in QI and healthcare systems science, there is an opportunity to join the Learning Health Systems Training Program (LHSTP). This innovative program is designed to equip trainees with advanced skills in data science and health systems research. Through the LHSTP, fellows learn to access and interpret patient- and clinician-level data from Duke’s Learning Health System, apply analytic methods to answer real-time clinical questions, and integrate their findings with the existing literature to drive meaningful improvements in care delivery. The LHSTP prepares fellows to become leaders in using data to inform practice and solve complex clinical problems.






